Hypermobility
Hypermobility is a condition that effects 10 to 20 percent of the population; the non medical term is ”double jointed”, and it may be present in one, or multiple joints. There is a strong genetic component to hypermobility, when I ask people about their mobile joints, they often tell me that their mother and siblings are all the same. Although it”s possible to become hypermobile in specific joints from doing yoga or gymnastics, the majority of people are born with this condition. There is some evidence emerging that hypermobility may be related to the shape of the bones, in particular the sockets. A more shallow socket will allow for greater mobility, and a deeper socket will provide greater stability. This makes sense to me, and it explains why people with hypermobility can pop their bones in and out.
Many famous yoga teachers are hypermobile, as it is their hypermobility that allows them to do deep backbends, and put their legs behind their heads. However, people who are hypermobile are more likely to injure themselves, and their injuries are slower to heal because their collagen fibers are weak to begin with. In a hypermobile person, the collagen fibers that are the building blocks of ligaments, tendons, walls of arteries, linings of organs, and between all the muscle fibers, are weak and loose, as opposed to dense and strong.
The most current research as sited by Thomas Myers is indicating that a persons mobility is determined by the number of fibroblasts. Fibroblasts are cells that excrete collagen into extracellular matrix. If a person has more of these cells in their body they will produce more collagen, which makes the tissues such as ligaments and tendons more dense and strong.
This video excerpt is of a fibroblast moving through the extracellular matrix leaving behind collagen excretions, you will observe that the trail of collagen is more dense.
We might conclude that people who are hypermobile and able to do crazy contortions with their bodies have fewer fibroblast cells, therefore less collagen. The pain associated with hypermobility can sometimes be confused with fibromyalgia, and the sleepless nights because of this pain can lead to chronic fatigue syndrome, and then be misdiagnosed.
Other symptoms associated with hypermobility include conditions that effect the connective tissues of the body such as:
- easy bruising, scarring that is stretched, stretch marks that appear at a young age, skin that feels soft and velvety
- weakness of abdominal and pelvic floor muscles leading to hernias
- unexplained chest pain and heart murmurs. blackouts, or near blackouts associated with change of posture
- bloating
- shortness of breath, perhaps diagnosed with asthma but not responding to inhalers
- anesthesia is ineffective, requiring much higher dosages
- severe fatigue
The Brighton hypermobility score (OR click here) helps people to determine their degree of hypermobility. If you score higher than 4 points you are considered hypermobile by medical standards, however it is still possible to be hypermobile in a joint that is not tested, i.e., your hips or lower back. For each of the following movements you get one point if you can do the action, one for each side of the body, left to right, and double points for both.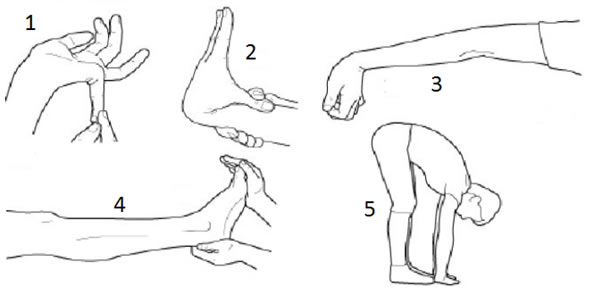
- Bend thumbs to forearm
- Bend little finger backwards to beyond 90 degrees
- Keep the arm straight and hyperextend the elbow backwards more than 10 degrees
- With straight legs bend the knee back more than 10 degrees
- Hands on floor, knees straight
In one of my previous blogs I wrote about labrum tears; they are far more common in people who are hypermobile in their hip joints. Our sense of proprioception tells the brain where the body is in space, but people who are hypermobile have fewer of these sensors, and so are less able to feel sensations coming from their joints.
Therapy for hypermobile people should be focused on strength building, with a balanced approach to stretching. Developing propriopception in the joints in smaller ranges of motion is also very beneficial to people with hypermobility. That translates into doing smaller movements, with more repetition, as opposed to going to an extreme range of motion and holding.

Recently I heard about a woman who was hypermobile, and her hip joint popped during an assist in a forward bend. She was already in a deep forward bend, and did not need an assist, but got one anyway. The teacher, who was hypermobile himself, knew how to get the femur to pop back in, and did an adjustment on her on the spot. Had that teacher not known what to do, the woman would have ended up in the emergency room. As it was, she was in pain for about a week afterwards. The concern with this constant popping and clicking of joints is the wear and tear it creates in the joint; there is strong evidence indicating that this could lead to arthritis.
After teaching yoga for almost 20 years, my understanding of hypermobility is finally sinking in. Contrary to what I used to think, I now believe that although a beautiful yoga pose remains beautiful, often that pose is only accessible to the hypermobile student, and people with normal mobility should not be encouraged to think that they will one day become hypermobile.
I remember one of the first times I went to an ashtanga mysore style class in New York, the teacher told me that he would have me taking my legs behind my head by the end of the week. I believed him. At the end of the week I was no closer to taking my legs behind my head, but I was very sore in all my muscles and joints from trying. For the next 10 years I tried almost every day to take my legs behind my head. I did get a little closer, but it hurt a lot and always seemed very unnatural. Why did I keep trying? I was trying to do the primary series of ashtanga yoga, and halfway through the series you”re supposed to take your legs behind your head. It was that simple. I wanted to be like other yogi superstars, most of whom are hypermobile in some, if not all of their joints. One of my favourite superstar yoga teachers has had serious problems with his sacroiliac joint from his hypermobility.
There is some controversy in the yoga community about hyperextension in the joints. I have encountered some teachers who believe that hyperextention in the knees and elbows is normal for some people, and not problematic for them. I have also spoken to many people who started yoga hypermobile, got even more mobile, and then started to have pain in their joints. It may not happen to everyone with hypermobility, but it is common enough that most yoga teachers are on the look out for hyperextension. Pulling hypermobile students out of hyperextended poses is not easy, because that person does not have normal proprioception. In their case they can”t feel the joint position; to them, hyperextended feels straight, and straight feels bent. Bringing a person out of hyperextention will require that their muscles work much harder to support them. Because people with hypermobility are more prone to injury, strengthening the musculature will help to stabilize and reduce injuries.
There is a type of therapy that involves injecting a slaine solution into weak ligaments that stimulates the ligament to heal itself by creating scar tissue, it”s called prolotherapy. CHECK OUT THE VIDEO BELOW Ross Hauser, MD is Medical Director of Caring Medical in Chicago land, specializing in Prolotherapy for tough cases of sports injuries and full body chronic pain. In this video, he reviews how…
TRIANGLE POSE: In the first image, Audrey looks like she is in a beautiful full expression of the pose, but upon closer examination you notice that her knees are hyperextended. I asked her to shorten her pose and microbend her joints; she found this much harder to do than the ”full expression of the pose”.

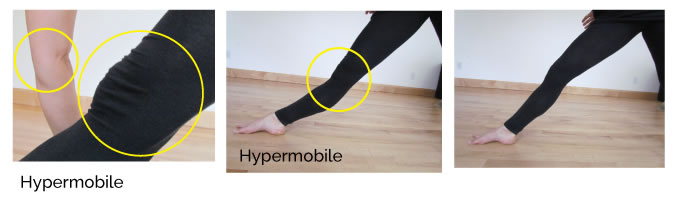
DOWNWARD FACING DOG POSE IMAGES: Audrey has been told many times to pull in from her low ribs, which unfortunately does not address the main issue with this pose; the hyperextension in the shoulders. To reorganize her posture I had Audrey shift her weight forward into her arms, much more than she wanted to initially. It made her work her upper body more, she was also unable to hyperextend her elbows in the balanced version of the pose. In the end she found the necessary muscular supports, which will eventually get stronger, and begin to feel natural.


HYPEREXTENDED ELBOWS: Ironically students with hypermobility will often have a constant need to stretch. The reason for this is that they often have achy joints, and think that more stretching is going to make them feel better. This becomes a vicious cycle, whereby more stretching = more mobility = equals more discomfort. Yoga teachers need to be aware of this situation, and ask their hypermobile students if they have any achiness in their joints. This type of student would benefit not only from reorganizing how they do each posture, but also from strength building practices off the mat. This is not the type of advice yoga teachers typically give their yoga students. In the old days I discouraged people from going to the gym because it would tighten them up. How little I knew then!

We appreciate ”Audrey Simard from BE Yoga”, helping us out by demonstrating for the photos.
Thanks for reading and please share the information with all your yoga teaching friends. Lets continue to raise the bar of knowledge, and support one another as we evolve as yoga teachers and healers.



